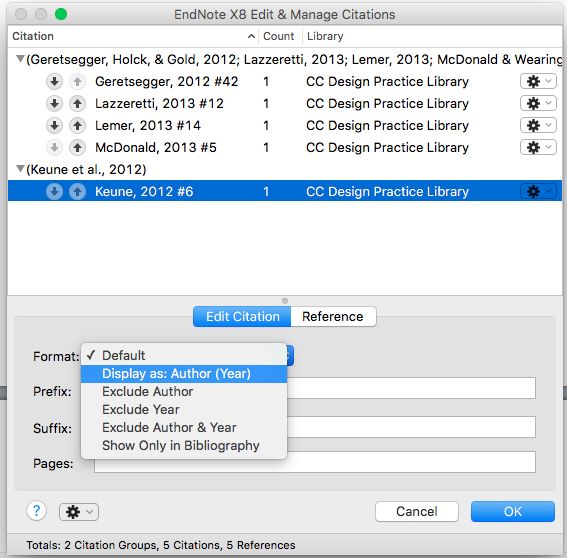 
Outcome measures included new opioid users per 1000 health plan enrollees per month and mean days’ supply of the opioid prescription per month. Patients could be counted again as new users if there were subsequent opioid claims that occurred 180 days or more apart. Patients were considered opioid naive if there were no other opioid prescription claims in the preceding 180 days. We included single-entity and combination products of oral opioid formulations. We analyzed pharmacy prescription claims for opioids dispensed from January 2015 through March 2019 from a single health plan serving more than 45 000 employees of a large Florida employer. This study follows the Standards for Quality Improvement Reporting Excellence ( SQUIRE) reporting guideline. This study was approved by the institutional review board at the University of Florida and was exempted from informed consent requirements because data were deidentified. Shared Decision Making and Communication.Scientific Discovery and the Future of Medicine.Health Care Economics, Insurance, Payment. 
Clinical Implications of Basic Neuroscience.Challenges in Clinical Electrocardiography.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
